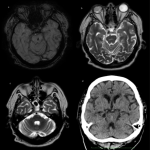
We have included several examples of common and uncommon etiologies of CMH in individuals of varying ages from our centre.
- 70-year-old with new onset of expressive aphasia and rapid cognitive decline. MRI depicts multiple CMHs at cortical and grey-white matter junction of both cerebral and cerebellar hemispheres, bilateral basal ganglia and pons. Differential diagnoses are chronic hypertensive encephalopathy and/or cerebral amyloid angiopathy.
- 70-year-old. CT brain demonstrated brainstem hyperdensity. MRI brain shows several CMHs of brainstem, may represent chronic hypertensive encephalopathy and/or cavernomas, capillary telangiectasia.
- 1-week-old. Multiple CMHs scattered in bilateral cerebral hemispheres. Our diagnosis is multiple cavernous malformation. Familial multiple cavernous malformation syndrome needs to be considered. Family counselling and genetic testing results are pending.
- 37-year-old with history of pineal germinoma post-surgery and radiotherapy. Multiple CMHs scattered in bilateral cerebral and cerebellar hemispheres. These may represent Radiation-induced cerebral vasculopathy.
- 22-year-old, admitted to hospital for severe diabetic ketoacidosis and developed status epilepticus in ward. Multiple CMHs are present predominantly at the grey-white matter junction of bilateral cerebral and cerebellar hemispheres, basal ganglia, corpus callosum and brainstem.
Cerebral Amyloid Angiopathy (CAA) and Hypertensive Microangiopathy
The anatomical distribution of the CMH is crucial to establish accurate diagnosis, whether CMH are located in deep versus lobar or superficial, as well as supratentorial versus infratentorial location.
CMH depicted in the basal ganglia, pons and cerebellum could be identified in hypertensive small vessel disease.
Although both hypertensive microangiopathy and CAA can demonstrate lobar CMH, the CMH in superficial location only are usually related to CAA. Some individuals may exhibit mixed lobar and deep patterns.
CAA could be attributed to β-amyloid protein deposition in cortical, subcortical and vessel wall in leptomeninges. CAA occurrence is mostly sporadic, but several familial forms of CAA have been recognized. Hereditary types of CAA are rare, show earlier onset and more severe in presentation.
CAA has been associated with development of Alzheimer’s disease. Presence of cortical superficial siderosis is prevalent in patients with CAA as well.
Patients with hypertensive microangiopathy or CAA may show symptoms of neurological deficits, cognitive impairment or macroscopic intracranial bleed.
Boston Criteria 2.0 was published in year 2022 to facilitate the diagnosis of CAA. This criteria is inclusive of clinical, radiological and pathological findings, which is established on the original Boston criteria (year 1995) and Modified Boston criteria (year 2010).
Cerebral Cavernous Malformations
Cerebral Cavernous Malformations (CCM) are groups of abnormal low-flow, thin- walled small vessels without normal intervening brain tissue, which could be found in brain and/or spinal cord. CCM in supratentorial location is more common compared to infratentorial location. CCM could present as sporadic cases or familial form. The sporadic cases are more common. These cases are mostly asymptomatic and display solitary lesion. Some sporadic cases are associated with developmental venous anomalies (DVA).
Familial cerebral cavernous malformation syndrome (FCCM) is an autosomal dominant disorder and constitutes approximately 20% of all CCM cases. About 20% to 50% of the individuals with FCCM are asymptomatic, with incidental findings of multiple CCM, predominantly on MRI brain. Most of the patients with FCCM displayed symptoms during second and fifth decades of lives. However, it is not uncommon for FCCM patients to manifest symptoms during childhood, which is earlier compared to sporadic form. Common symptoms include fitting episodes, focal neurological impairment, cerebral bleed and headache. The number of lesion in CCM patients may increase progressively at a rate of 0.2 to 0.4 lesions per patient-year.
Suspicion of FCCM is raised if there are five or more CCM exhibited in a patient, with involvement of at least two family members, as well as genetic mutations in one of the three genes resulting in FCCM. The 3 genes responsible for FCCM are KRIT1, CCM2, and PDCD10 (locus CCM1, CCM2 and CCM3).
Adjacent hemosiderin deposition and gliotic changes are frequently depicted, due to thrombosed vessels or microbleed.
CCM can be classified into 4 types by their MRI characteristics and histopathological features, according to Zabramski et al and additional Type V proposed by Nikoubashman et. al for CCM with gross extra-lesional bleed in non- radiation induced cavernous malformation.
Radiation- induced microhemorrhages
Cranial radiation therapy has been used to treat many primary brain neoplasms and metastatic brain tumours.
Cranial irradiation may cause endothelial dysfunction, resulting in disruption of blood-brain barrier and vascular damage, such as telangiectasia, cavernoma or aneurysm formation, small arteriolar dilatation and vessel wall thickening. Cerebral ischemia and intracranial haemorrhage, including microhemorrhages, may occur as late complications.
Multiple studies have shown that patients who have history of cranial radiotherapy show higher risk of developing CMH. These CMH were detected on SWI sequence during surveillance MRI brain. It was learnt that the amount of CMH may increase gradually each year, following cranial irradiation. Studies also depicted that radiation dose has positive correlation with occurrence of CMH, especially in those individuals receiving radiation dose of at least 30Gy. These patients who developed CMH post cranial radiotherapy may suffer from potential cognitive impairment as well.
Acute haemorrhagic leukoencephalitis (AHLE)
AHLE is also known as Hurst disease. It is an uncommon and severe type of demyelinating disease, which is usually preceded by viral infection. There is a resemblance between AHLE and acute disseminated encephalomyelitis (ADEM) in the clinical course. Hence, AHLE is always considered to be in the same spectrum as the ADEM. ADEM usually occurs in children, whereas AHLE usually involves adult patient. Literature review depicts male predominance of 67% in AHLE. Patients with AHLE would present with fast neurological impairment, resulting in unconsciousness and demise. Mortality rate for AHLE is high, from 46.5% upto 70% in some literature. Patients who survived may suffer from long-term neurological deficit.
MRI brain of patients with AHLE demonstrate confluent white matter changes, mass effects, cerebral oedema as well as microhaemorrhages. The presence of cerebral haemorrhage is helpful in differentiating AHLE from ADEM.